How Does Dental Bone Grafting Work? Your Guide
If you’ve been told you need a bone graft before getting dental implants, the reaction is usually the same. Frustration first, then questions. You came in expecting to replace a missing tooth, and instead you heard that the bone underneath it isn’t strong enough yet.
That doesn’t mean implants are off the table. It means the foundation needs help.
A lot of adults in Austin, Georgetown, Round Rock, Cedar Park, Wells Branch, and Liberty Hill find themselves in this exact spot after a tooth extraction, advanced gum disease, or years of wearing a gap in their smile. The good news is that modern bone grafting is designed to rebuild the support an implant needs. With today’s 3D imaging, digital planning, and precise surgical techniques, the process is far more predictable and understandable than is commonly assumed.
Your Trusted Dentist for Dental Implants in Austin and Georgetown TX
One of the most common implant conversations starts with disappointment. A patient searching for dental implants near me or a dentist near me comes in ready to fix a missing tooth, only to learn there isn’t enough jawbone to hold an implant securely.
That’s not a dead end. It’s a planning issue.
When a tooth has been missing for a while, or when gum disease has affected the supporting structures around the teeth, the jaw often loses the shape and density needed for a long-lasting implant. Bone grafting is the procedure used to rebuild that area so the implant has a stable base.
Why this diagnosis surprises people
Jawbone loss is often not visible to the individual. They may notice a loose denture, a shifting bite, or a space that seems harder to restore than expected, but they don’t always connect those changes to the bone itself.
That’s why an implant evaluation matters. A modern dental office doesn’t guess. It studies the site carefully, measures the available bone, and plans the treatment around what will support the final restoration properly.
“You’re not a candidate yet” often really means “you need the foundation rebuilt first.”
Patients looking for a dentist in Austin, TX or dentist in Georgetown, TX usually want a clear answer, not a vague warning. The most reassuring explanation is also the most accurate one. Bone grafting works by helping your body create new support where support has been lost.
What patients want to know right away
Before they ask about cosmetic dentistry, crowns, or even the implant itself, individuals often want answers to a few practical questions:
- Why did the bone shrink
- How does dental bone grafting work
- Will the graft last
- How long before I can move forward with treatment
Those are the right questions. Bone grafting isn’t just an extra procedure. For many implant cases, it’s the step that makes a durable result possible.
Why Jawbone Loss Happens and Why It Matters for Your Smile
A patient comes in after losing a back tooth and feels fine. Chewing still works. The smile does not look much different. Then we review a 3D CT scan at 3D Dental in Austin or Georgetown and see the underlying issue. The bone in that area has already started to thin and collapse.
Your jawbone is active tissue. It stays healthy when it receives regular stimulation from tooth roots and remains free of ongoing inflammation. Change those conditions, and the bone begins to remodel in the wrong direction.
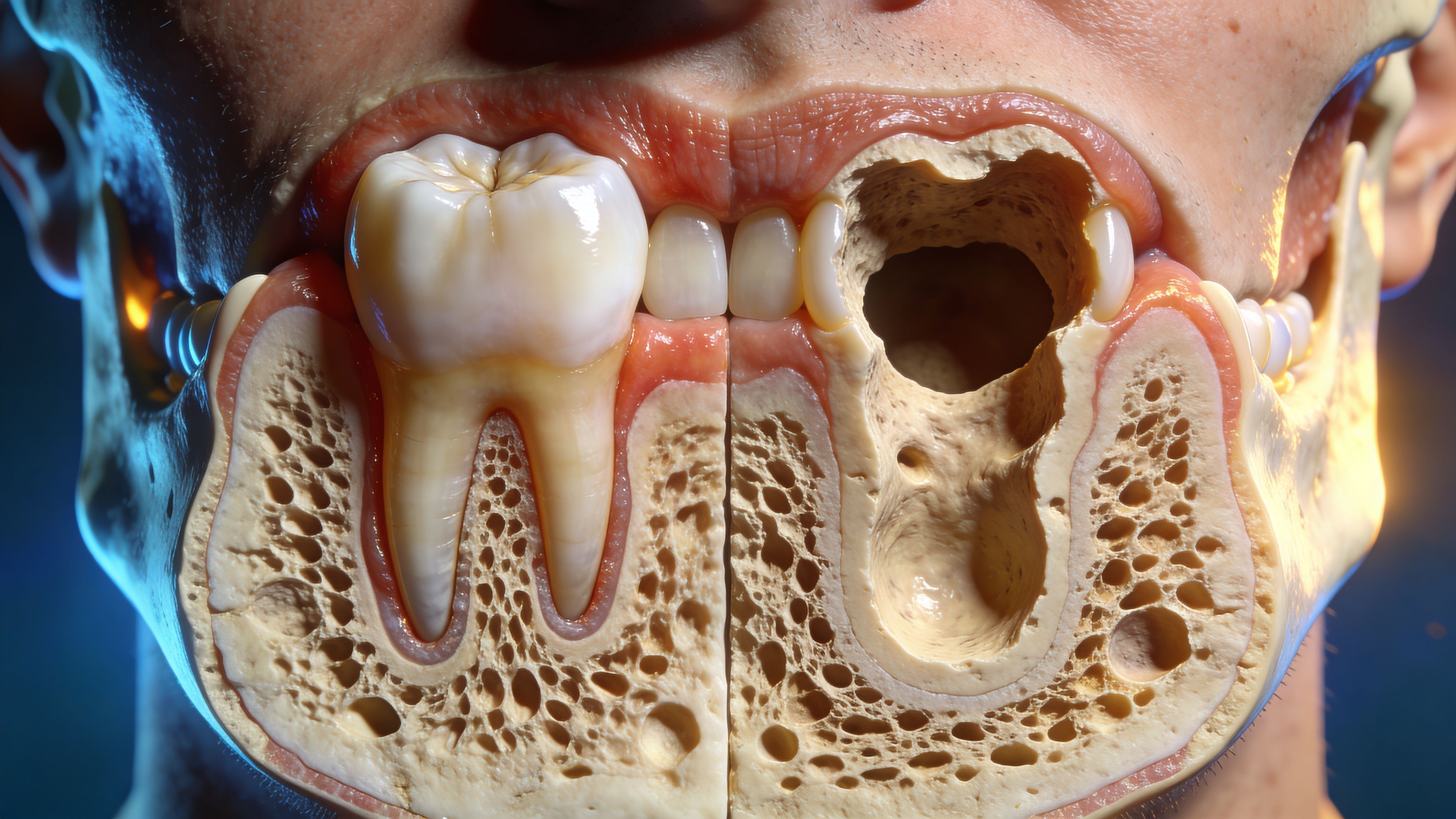
The most common reasons bone is lost
The pattern is usually straightforward. A natural tooth root transmits pressure into the jaw every time you bite. Remove the root, and the body no longer has the same reason to maintain that bone volume.
Bone loss often follows:
- Tooth extraction, especially if the site is not preserved at the time of removal
- Periodontal disease, which can destroy the bone that supports teeth
- Long-term missing teeth, because unused areas tend to resorb over time
- Trauma or fracture, which can leave the ridge narrower or irregular after healing
The rate and severity are different for every patient. Some lose width first. Others lose height, density, or both. That difference matters because implant planning depends on precise measurements, not rough estimates. At 3D Dental, we use 3D CT imaging to map the exact shape of the site so treatment is based on what is present.
Why bone loss affects more than one missing tooth
Patients often expect the problem to stay confined to the empty space. In practice, bone loss can affect the way the whole area functions and looks.
As the ridge shrinks, several things can happen:
- Implant placement gets more complex because there may not be enough bone for ideal position and stability
- Facial contours can change because the jaw supports the lips and lower face
- Adjacent teeth can face more stress if gum disease or bite imbalance is part of the picture
- Chewing patterns may shift when patients avoid one side and overload the other
Time matters here.
The longer a site sits without a root or a well-planned replacement, the more likely it is that treatment will require grafting, contour correction, or a staged approach instead of a simpler implant procedure.
Why this matters for your smile
Jawbone loss is not only a structural issue. It can change the final appearance of the restoration.
If the bone and gum support are reduced, the replacement tooth may need to be positioned differently or shaped to compensate for missing volume. In the front of the mouth, that can affect smile symmetry. In the back, it can affect bite strength and long-term wear. Good implant dentistry starts with the foundation because the foundation affects both function and appearance.
That is where modern planning makes a real difference. With in-house digital design, 3D printing, and CT-guided treatment planning, we can evaluate whether a site should be preserved, rebuilt, or restored right away. Patients get a clearer answer, and the result is more predictable, more precise, and more comfortable than the old model of placing implants with limited imaging and guesswork.
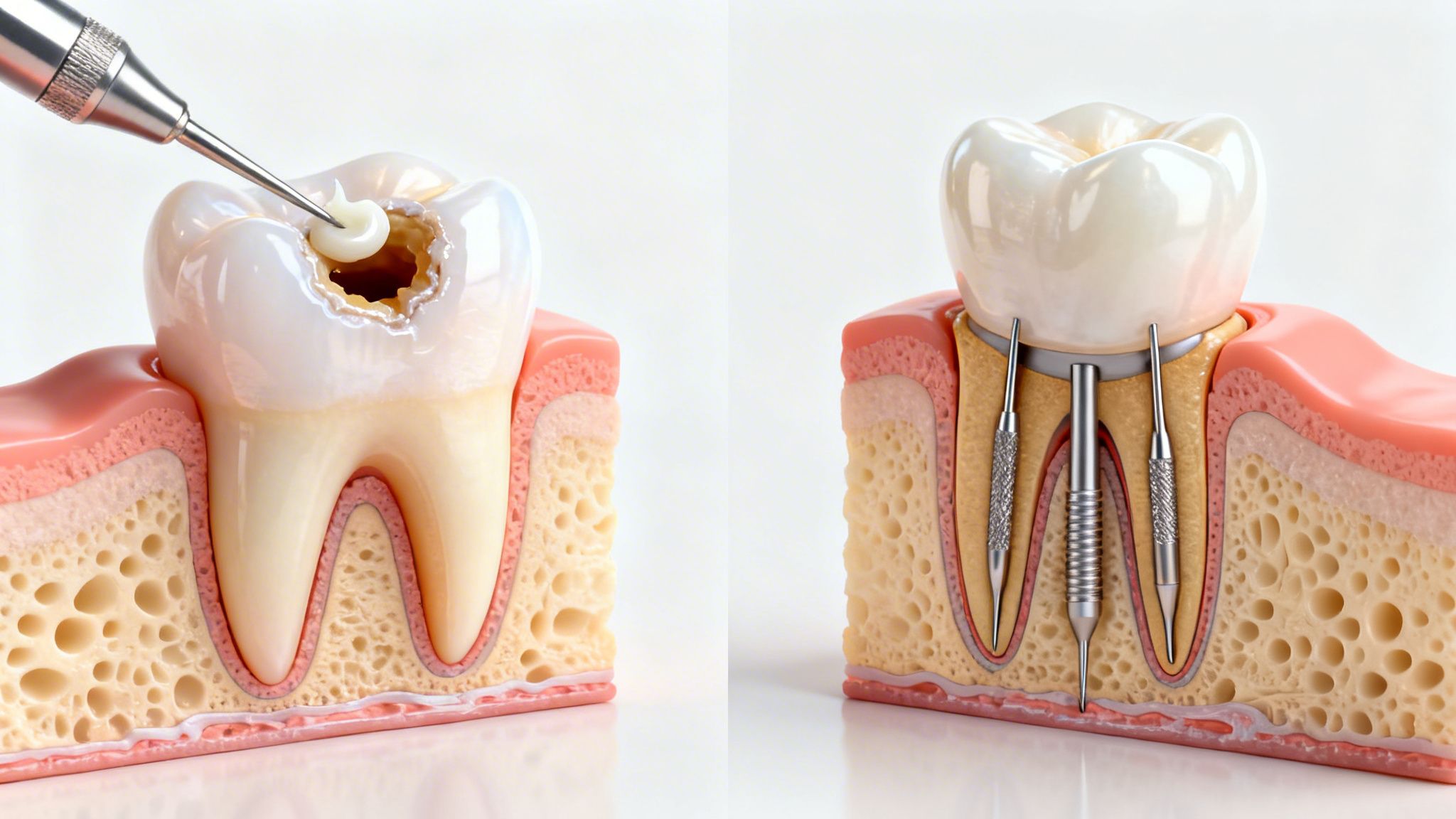
How a Dental Bone Graft Biologically Rebuilds Your Jawbone
A dental bone graft rebuilds your jaw by creating a protected space where your body can grow new bone. The graft material holds volume, supports blood vessel growth, and gives bone-forming cells a place to attach while the area heals.
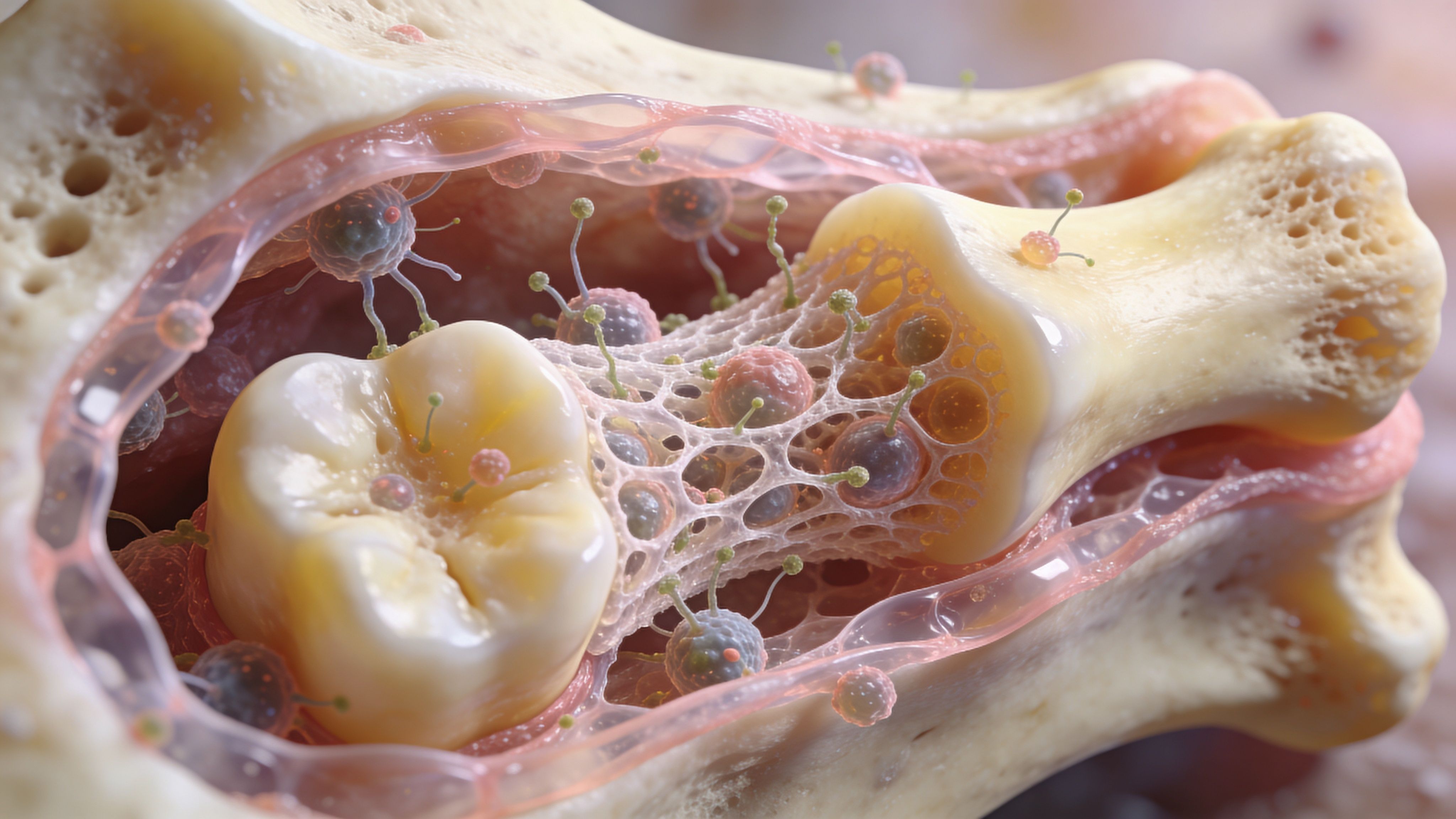
The basic biology in plain English
Three biologic processes drive graft healing.
- Osteoconduction means the graft acts as a framework for new bone to grow across
- Osteoinduction means the healing environment signals the body to recruit bone-building cells
- Osteogenesis means living bone is actively formed as the site matures
Patients do not need to memorize those terms. What matters is the sequence. We place a graft into an area that has lost volume, stabilize it, protect it from pressure and soft-tissue collapse, and let your body replace that scaffold with stronger natural bone over time.
At 3D Dental, that process starts before treatment begins. With 3D CT imaging, we can measure the width, height, and shape of the defect instead of estimating it from a two-dimensional X-ray. That matters because a narrow ridge, a contained socket, and a larger horizontal defect do not heal the same way and should not be grafted the same way.
Guided bone regeneration
Many grafting procedures use guided bone regeneration, or GBR. In this approach, the graft is placed where bone is missing and covered with a barrier membrane that helps maintain space for bone to grow.
The membrane has a practical job. It helps keep faster-growing soft tissue from filling the area before bone has time to develop. If that space is lost early, the site can heal smaller than planned, which affects implant positioning later.
Good GBR depends on details patients usually never see. The graft has to fit the defect. The membrane has to stay stable. The tissue closure has to be tension-free so the area stays covered during healing. Those technical points are a big reason results vary from office to office.
Our in-house lab and 3D printing workflow help here. When a case needs a more precise surgical plan, we can use your CT scan to design guides and visualize the defect in advance, which improves graft placement and reduces guesswork during surgery.
Here’s a visual overview of how that process works in practice:
What happens after placement
After the graft is placed, the body moves through a predictable healing pattern. First, the area forms a stable blood clot and starts the early inflammatory phase. Next, new blood vessels grow into the site and bring in the cells that support repair. Then the graft slowly remodels as immature tissue is replaced with more organized, stronger bone.
This part takes patience.
Some grafts mature faster than others. Small socket preservation cases often heal more easily than larger ridge defects, sinus grafts, or sites that have been missing a tooth for years. Smoking, uncontrolled diabetes, active gum disease, and excess pressure on the area can also slow healing or reduce the amount of regenerated bone.
What improves long-term graft durability
Long-term success is not only about whether a graft "takes" in the short term. The ultimate goal is durable bone volume that can support an implant in the right position and keep supporting it under bite forces for years.
That is why we focus on planning, containment, and follow-up. A graft placed in the correct dimension and allowed to heal fully is more likely to give stable implant support than a rushed case with limited imaging. At 3D Dental in Austin and Georgetown, we verify healing with modern imaging when needed, evaluate whether the site has matured enough for implant placement, and make decisions based on the biology in front of us, not on a fixed one-size-fits-all timeline.
Some patients are candidates for grafting and implant placement close together. Others get a better result with a staged approach. The trade-off is time versus predictability, and in many cases, choosing the slower path produces the stronger long-term foundation.
Understanding the Different Types of Bone Graft Materials
Material choice affects how a graft handles space, how quickly it remodels, and how much support it gives an implant later. It also affects the treatment plan. A small extraction socket often allows more flexibility than a thin ridge that has been shrinking for years.
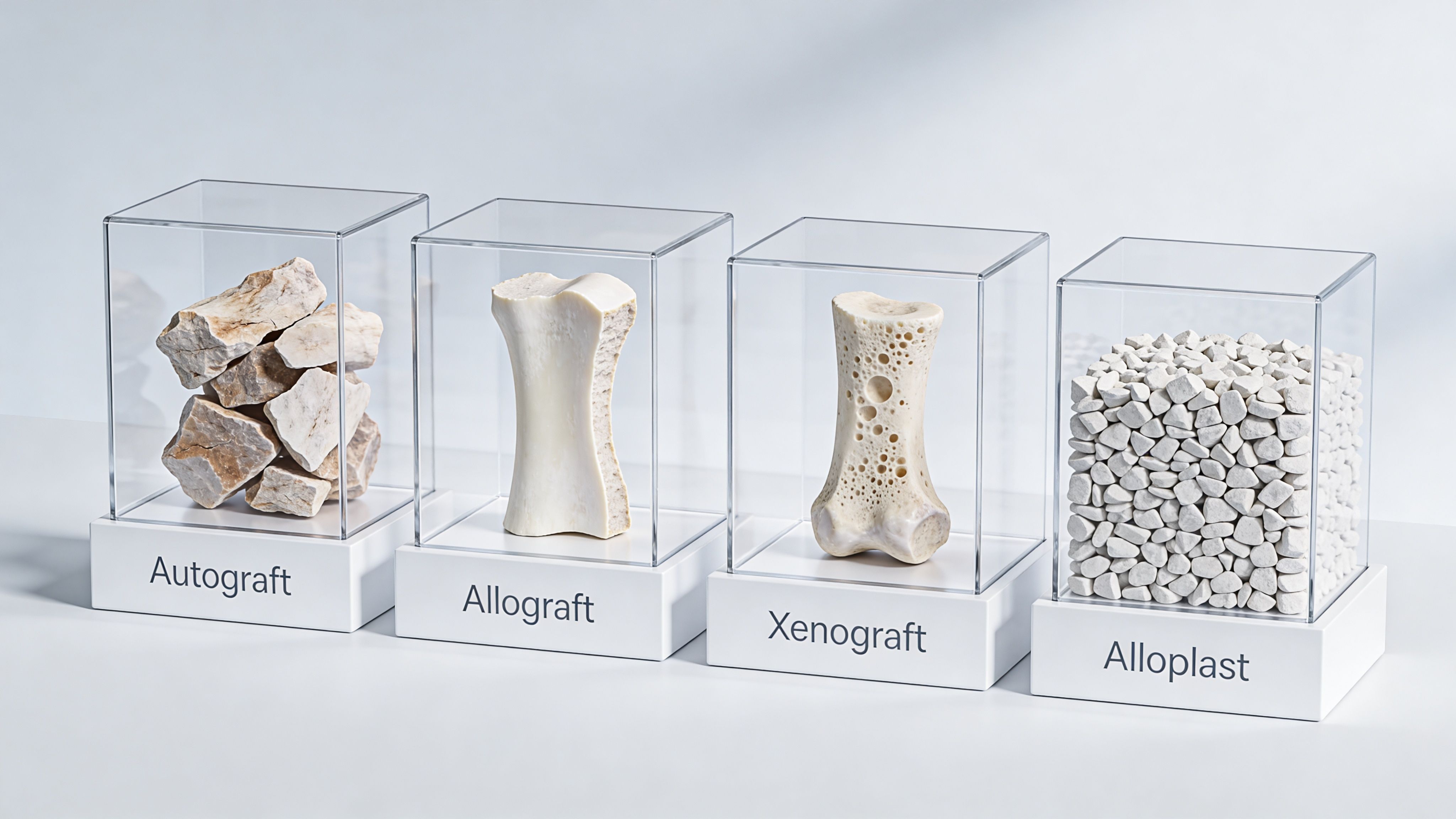
At 3D Dental in Austin and Georgetown, we do not pick a graft by label alone. We match the material to the defect shown on the 3D CT scan, the amount of missing width or height, the timing of the future implant, and the patient’s preferences. That planning matters because the right material for socket preservation may not be the right material for a larger ridge rebuild.
The four main categories
Bone graft materials generally fall into four groups:
| Graft type | Where it comes from | Why it may be chosen | Main trade-off |
|---|---|---|---|
| Autograft | Your own bone | Excellent biologic compatibility and strong healing potential | Requires bone to be taken from another site |
| Allograft | Human donor tissue | Avoids a second surgical site and works well in many routine grafts | Remodels differently than your own native bone |
| Xenograft | Animal-derived material | Holds space well and can be useful where structure matters | Some patients do not want an animal-based material, and turnover can be slower |
| Alloplast | Synthetic material | No human or animal donor source, useful in selected defects | Performance depends heavily on matching the material to the case |
How we choose between them in real cases
Autograft uses your own bone. It has strong healing potential, but the trade-off is straightforward. Treatment becomes more involved because bone has to be collected from another area. In a limited defect, that added surgery may not be worth it. In a more demanding site, it can be a smart choice.
Allograft is commonly used because it avoids that second donor site. For many patients, that means a simpler procedure and a smoother recovery while still giving us a scaffold the body can replace with living bone over time.
Xenograft is often chosen when we want the graft to maintain shape and volume longer. That can be helpful in areas where space maintenance is a priority, especially if the bone wall is thin. The trade-off is slower remodeling.
Alloplast is the synthetic category. Some patients prefer it for personal or religious reasons. Some defects respond well to it. Others do better with a material that remodels in a different way. Selection has to be precise.
The best graft material is the one that fits the defect, the restorative plan, and the patient’s priorities.
Technology improves the material decision
The material matters. The fit between the material and the defect matters more.
A 3D CT scan shows whether the problem is loss of width, height, or both. Our in-house lab and digital planning workflow help us decide how much graft volume is needed and where implant support must be strongest. In more advanced cases, 3D printed guides and models help translate that plan accurately to the surgical site. That level of planning reduces guesswork and helps us avoid overbuilding, underbuilding, or choosing a material that is stable in the wrong dimension.
Patients usually ask which graft lasts the longest. The better question is which graft is most likely to heal into durable bone for the restoration being planned. A slower-resorbing material can be useful in one case and less ideal in another. A faster-turnover material can be helpful when we want more active remodeling before implant placement. Long-term success depends on how the material, the defect, the blood supply, and the implant plan work together.
Material is only one part of success
A well-chosen graft can still fail if the site is not managed carefully.
Outcome also depends on:
- How cleanly the site is prepared
- Whether the graft is protected with the right membrane when needed
- How well the area is closed and kept stable
- How much healing time the site needs
- Whether the future implant is planned in the correct position from the start
That is why we plan bone grafting and implant placement as one connected treatment, not as separate decisions. In modern implant dentistry, the goal is not merely to place graft material. The goal is to rebuild the right foundation, in the right shape, for a restoration that lasts.
Your Bone Grafting Procedure Step by Step at 3D Dental
You come in expecting a complicated surgery. In most cases, the appointment feels far more controlled than patients anticipate because every decision has already been mapped out before treatment starts.
At 3D Dental in Austin and Georgetown, bone grafting is planned as part of the full implant process, not as an isolated procedure. We use the scan, the digital records, and the future tooth design to decide exactly what the site needs and what it does not. That approach helps us keep treatment precise, efficient, and comfortable.
Step 1. Diagnose the site with 3D imaging
The first step is a close clinical exam followed by 3D CT imaging. A regular dental X-ray can suggest bone loss. A CT scan shows the shape of the defect in three dimensions, including the width of the ridge, the available height, and the nearby anatomy we need to protect.
That matters because bone loss is not one-size-fits-all. Some sites need socket preservation after an extraction. Others need targeted ridge rebuilding before an implant can be placed in the right position. With a clear scan, we can explain the problem in concrete terms and show you the plan on screen.
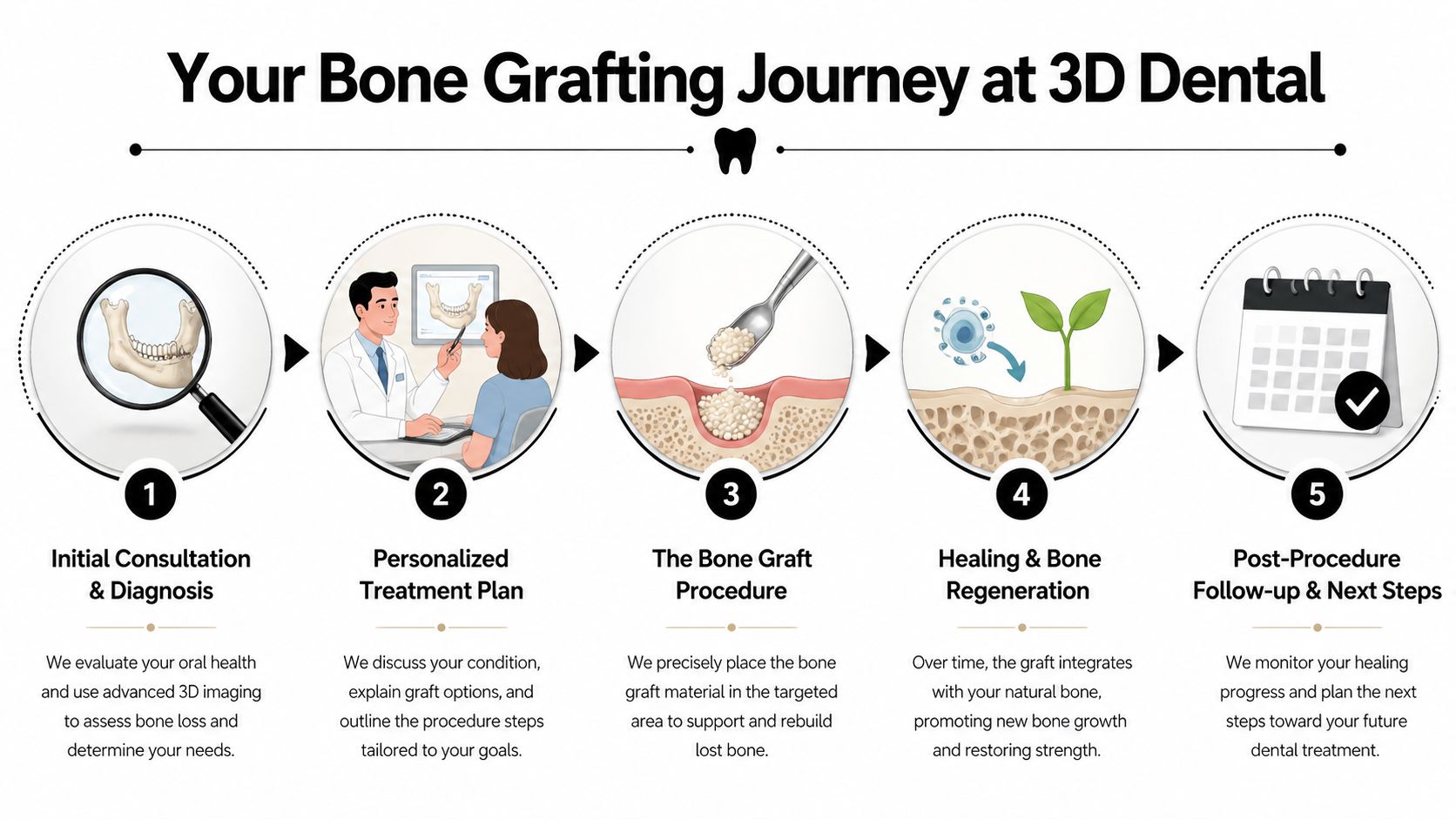
Step 2. Build the surgical plan before the appointment
Once we know the defect, we choose the grafting method, timing, and materials based on the final restoration. That planning stage is where advanced technology improves predictability.
Our team can combine CT data with digital scans and, when useful, use our in-house lab and 3D printing to prepare guides or models that match the case. For patients, that usually means fewer surprises, cleaner execution, and a plan that is tied directly to implant position instead of general estimates. It also lets us have an honest conversation about timing, because a smaller graft and a larger reconstruction do not heal on the same schedule.
Step 3. Perform the graft with local anesthesia and careful site control
On the day of treatment, the area is numbed thoroughly so the procedure is comfortable. Sedation may also be discussed for the right patient and the right case. After the site is accessed, the area is cleaned and prepared, the graft material is placed where bone volume is missing, and a membrane is used when protection and stability are needed. Sutures then hold the tissue in a position that supports healing.
For many straightforward cases, treatment is completed in a single office visit. More advanced defects take more time and more technique. The trade-off is simple. A site that is rebuilt carefully gives us a better foundation for an implant that needs to function for years.
Step 4. Verify healing instead of guessing
The surgical visit is only one part of the process. We check the site during follow-up visits because soft tissue can look settled before the underlying graft has matured enough for the next stage.
That is one reason we plan bone grafting around the long-term result, not around speed alone. If implant placement is done too early, stability can suffer. If the timing is right, the rebuilt site is more likely to support strong integration and a better final restoration. Patients who want to understand the bigger picture often review our page on dental implant success rates and long-term outcomes.
Step 5. Transition to implant placement with the final tooth in mind
Once healing has progressed as expected, we move to implant placement or the next restorative phase. Because the graft, implant, and final tooth were planned together from the beginning, the transition is more accurate and more efficient.
Patients often notice a few practical differences at 3D Dental:
- 3D imaging that shows the defect clearly
- A treatment plan built around the future implant, not guesswork
- In-house lab and 3D printing support for better case coordination
- Careful follow-up before the site is loaded
- A more comfortable experience than many patients expect
That combination of planning, technology, and surgical discipline is what makes modern bone grafting feel less intimidating. The procedure itself is only part of the story. Its primary value is building the right bone, in the right shape, for a restoration that has a strong chance to last.
Healing Recovery and Long-Term Success Rates for Bone Grafts
A common moment in consults happens about a week after surgery. The soreness has eased, the tissue looks calmer, and the patient assumes the graft must be finished healing. In reality, the visible part often improves well before the bone underneath has matured enough for implant support.
That gap between feeling better and being ready is why recovery has to be managed with discipline. At 3D Dental, we do not rely on guesswork or the calendar alone. We use clinical follow-up and 3D imaging to confirm how the site is developing before we recommend the next step.
The healing timeline patients should expect
Bone graft healing happens in layers. Soft tissue closure comes first. The deeper process takes longer as blood supply develops, graft particles are remodeled, and your body replaces that material with living bone.
For many patients, daily comfort improves within the first one to two weeks. That is encouraging, but it does not mean the graft is ready to carry implant forces. Maturation often continues for several months, and the exact timeline depends on the size of the defect, the graft material used, your overall health, and whether the graft was done with an extraction or as a separate procedure.
Technology improves decision-making for patients. A 3D CT scan gives us a much clearer view of bone volume and healing progress than a basic two-dimensional image. In more complex cases, our in-house lab and 3D planning also help us compare the grafted site to the final restorative goal, so timing is based on what the bone can support, not on optimism.
What supports recovery
Recovery tends to go best when patients protect the site and let the biology do its work.
- Avoid pressure on the area, including chewing where we tell you not to chew
- Keep the site clean exactly as instructed, without overbrushing or disturbing the graft
- Attend follow-up visits so we can check healing before small issues become larger ones
- Control risk factors such as smoking, uncontrolled diabetes, active gum disease, or clenching
- Stay realistic about timing, especially if the graft has to rebuild significant lost bone
A quiet, comfortable recovery is a good sign. It is not proof that the graft is fully mature.
What long-term durability really looks like
Patients deserve a straight answer here. Bone grafting is highly predictable in the right case, but success is not automatic.
Long-term durability depends on the quality of the original defect, the graft design, blood supply, infection control, and whether the rebuilt site is allowed to heal fully before loading. That is why planning matters so much. At 3D Dental, we use 3D CT data from the start so we can measure the defect, choose the right approach, and build toward the implant position we want. If a case benefits from custom guidance or printed models through our in-house lab, that added precision can reduce surprises later.
The outcome patients care about is simple. Will this bone hold up well enough to support a stable implant over time? In many cases, yes. Properly planned grafted sites can go on to support implants very successfully for years. For a broader look at what affects implant predictability over time, read our review of dental implant success rates and long-term outcomes.
The trade-offs patients should understand
Bone grafting adds another phase of treatment. It can increase cost, healing time, and the number of visits. In some cases, it also means delaying the implant so the foundation can develop correctly.
That added effort often protects the final result. Without enough bone, an implant may need to be placed in a compromised position, or it may not achieve the stability needed for a restoration that looks right, feels comfortable, and handles bite forces well over time.
A good candidate is not only someone with bone loss. It is someone willing to treat the graft as part of the final implant plan, not as a shortcut on the way to it. That mindset, paired with careful imaging, in-house digital planning, and measured follow-up, is what gives modern bone grafting its best chance of lasting success.
Enabling Dental Implants and All-on-4 Restorations in Austin
People rarely seek bone grafting for its own sake. They seek it because they want something on the other side of it. They want to chew comfortably again, replace a missing tooth, stabilize a loose plan, or move forward with a full-arch restoration.
That’s why bone grafting should be viewed as enabling care. It creates the foundation that makes advanced implant treatment possible.
Why implants depend on bone quality
A dental implant needs enough bone volume and density to achieve stable osseointegration. When that support is missing, the implant can’t be placed in the ideal position or can’t be placed predictably at all.
That’s why bone grafting is often mandatory for long-term implant success, because it addresses insufficient jawbone that would otherwise prevent the implant from achieving stable osseointegration, according to the clinical overview of pre-implant grafting and implant stability.
How grafting opens more treatment options
A successful graft can support several types of restorative care:
- Single-tooth implants when one missing tooth needs a stable root replacement
- Multiple-implant cases where support has to be rebuilt across more than one site
- Implant bridges when spacing and load need to be carefully managed
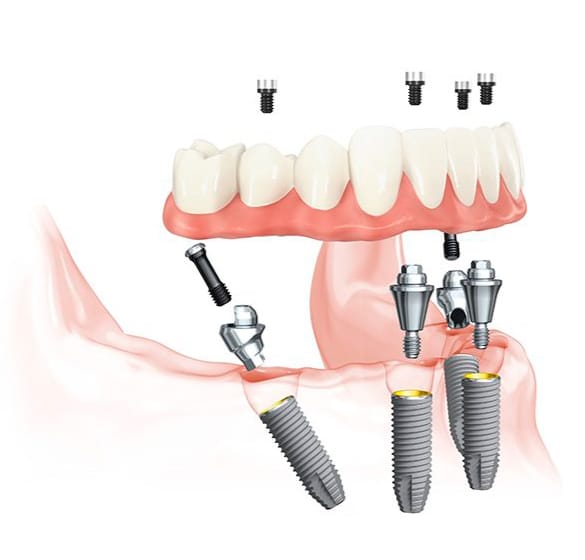
- All-on-4 treatment when a full arch requires precise planning around available bone
For patients considering full-arch care, this guide to All-on-4 dental implants in Austin explains how implant planning and full-mouth restoration fit together.
Why technology improves predictability
The best implant outcomes happen when the graft and the final restoration are planned together. That’s where advanced diagnostics make a real difference.
A 3D CT scan helps identify where bone is missing and where the future implant should ideally go. Digital scans help map the bite and the shape of the restoration. An in-house lab and 3D printing help translate that plan into surgical precision and a more coordinated restorative workflow.
The strongest graft isn’t just the one that heals. It’s the one that heals in the right shape for the tooth or arch that comes next.
For patients looking for dental implants near me, restorative dentistry, or a local office that can manage both the surgical and restorative sides of care, that integration matters. It reduces surprises and improves how the final smile looks, feels, and functions.
Schedule Your Bone Grafting Consultation at 3D Dental Today
If you’ve been told you don’t have enough bone for implants, the next step should be a detailed evaluation, not a guess. The right consultation answers what’s happening now, what can be rebuilt, and whether the timing makes sense for your smile.
At a modern implant visit, that usually starts with imaging and diagnosis. A 3D CT scan can show the exact shape of the bone, the amount of support that remains, and whether the area is ready for an implant, needs grafting first, or may benefit from a staged approach. That level of precision matters whether you’re searching for a dentist near me, a dentist in Austin, TX, a dentist in Georgetown, TX, or a practice that handles more advanced restorative care.
What your consultation should include
A strong consultation is clear and specific. You should expect:
- A full exam and imaging review so the site is measured accurately
- An explanation of your graft options based on your anatomy and treatment goals
- A timeline for healing and the next restorative steps
- A transparent cost discussion that includes available payment pathways
Patients also deserve practical convenience. That means support with insurance, realistic scheduling, and financing options that help move treatment forward instead of delaying needed care.
Why patients choose a tech-focused local practice
For adults in Austin, Georgetown, Round Rock, Cedar Park, Wells Branch, and Liberty Hill, convenience matters. So does having advanced care under one roof.
A practice with digital diagnostics, an in-house lab, and 3D printing can often make treatment planning more coordinated from the start. That doesn’t just make the process feel more efficient. It helps align the graft, the implant, and the final restoration in a way that’s easier to understand and easier to execute.
If you’re also looking for ongoing dental care, cleaning and exams, dental x-rays, new patient exams, cosmetic dentistry, teeth whitening, tooth extraction, or an emergency dentist, it helps to choose an office that can support both your immediate needs and your long-term treatment plan.
A straightforward next step
If you’re ready to find out whether a bone graft could make implants possible, schedule a consultation and get a real answer based on imaging, not assumptions. A good plan should leave you knowing what’s needed, why it matters, and what comes next.
If you’re looking for a modern, patient-first path to implants in North Austin or Georgetown, schedule a consultation with 3D Dental. The team offers advanced imaging, an in-house lab, flexible financing through Cherry and Sunbit, and complete care designed to make complex treatment feel clear, precise, and manageable.
Ready to get started?
Schedule a free, no obligation consultation with our team and see what's possible for your smile!
Georgetown
- Mon-Thurs8:30am-5pm
- Fri8am-3:30pm
- Sat-SunClosed
Austin
- Mon-Tues8am-5pm
- Wed-Thurs9am-6pmFri8am-2pm
- Sat-SunClosed



























































.jpg)
