How Long Do Dental Implants Last?

TL;DR: Dental implants are built to last. Research shows 95 to 97% survival over the first decade, including a pooled 96.4% survival rate at 10 years, and about 80% at 20 years, while fixed bridges often last 10 to 15 years and removable dentures 5 to 10 years. With good home care, healthy gums, and regular maintenance, implants can remain functional for decades and may last a lifetime.
If you're dealing with a missing tooth, you're probably not thinking only about appearance. You're thinking about chewing on one side, food getting trapped, shifting teeth, and whether the solution you choose will hold up years from now.
That question matters. A tooth replacement isn't just about filling a gap today. It has to stay comfortable, stable, and easy to live with over time. For patients searching for dental implants near me, a dentist in Austin, TX, or a dentist in Georgetown, TX, durability is usually one of the first concerns.
Your Guide to Lasting Dental Implants in Austin TX
A missing tooth changes more than your smile. It affects how you eat, how you speak, and often how confident you feel in everyday moments.
Many patients wait because they're unsure whether implants are worth it. They want something that feels permanent, but they also want honest answers about upkeep, wear, and long-term value.
Why implants are treated as a long-term solution
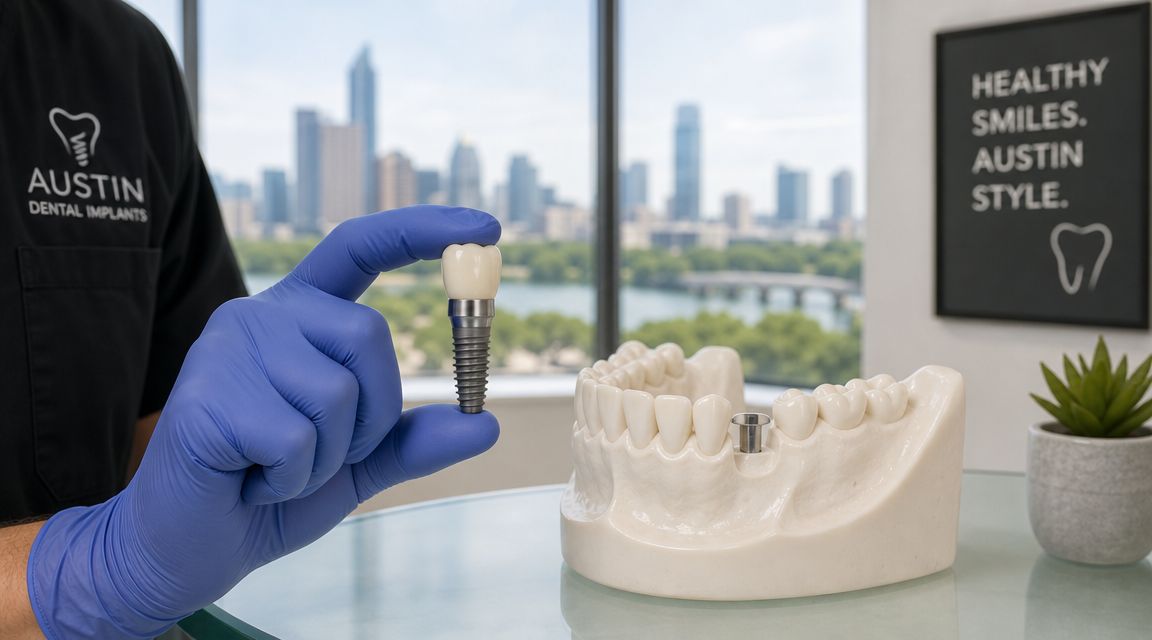
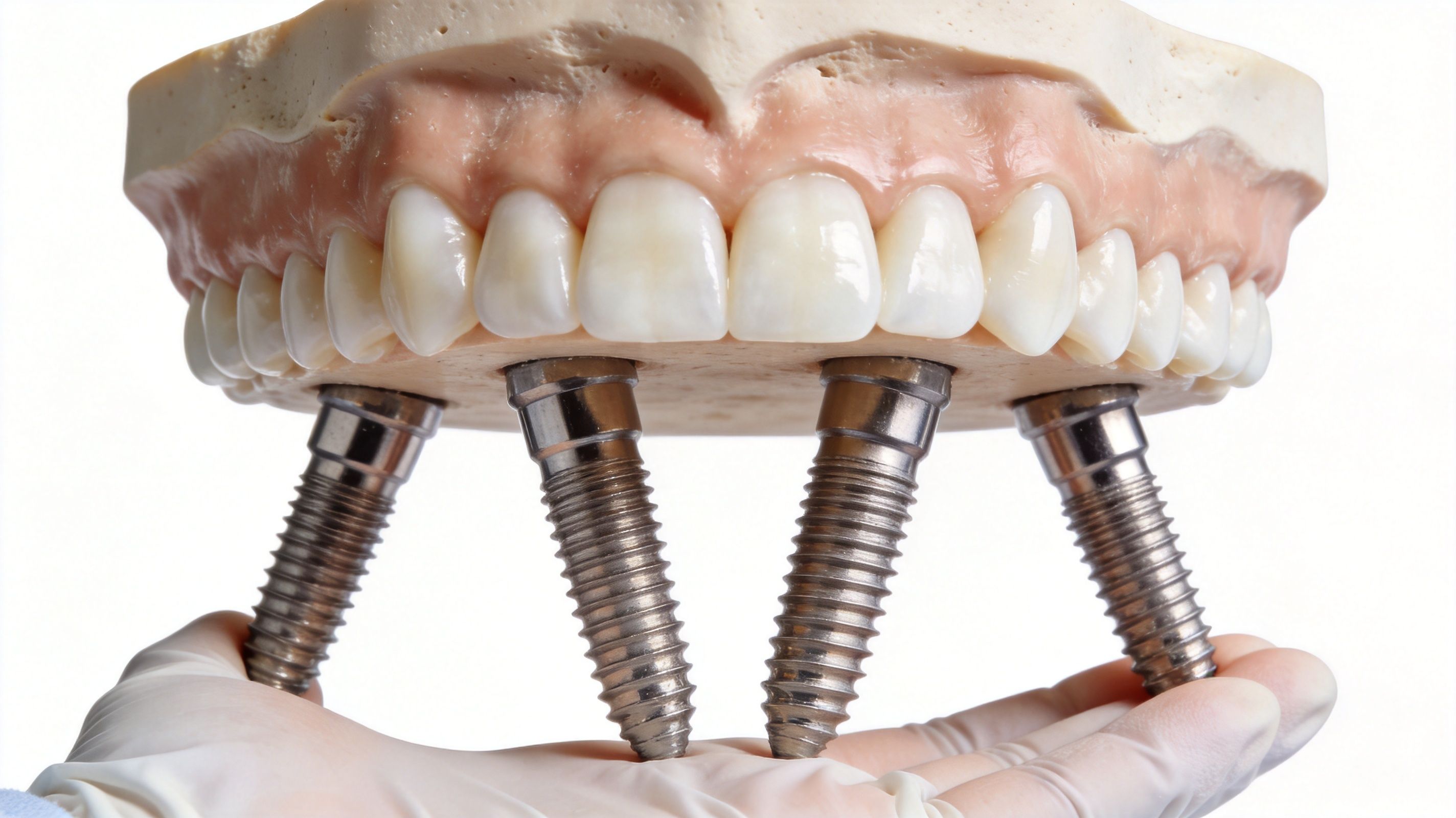
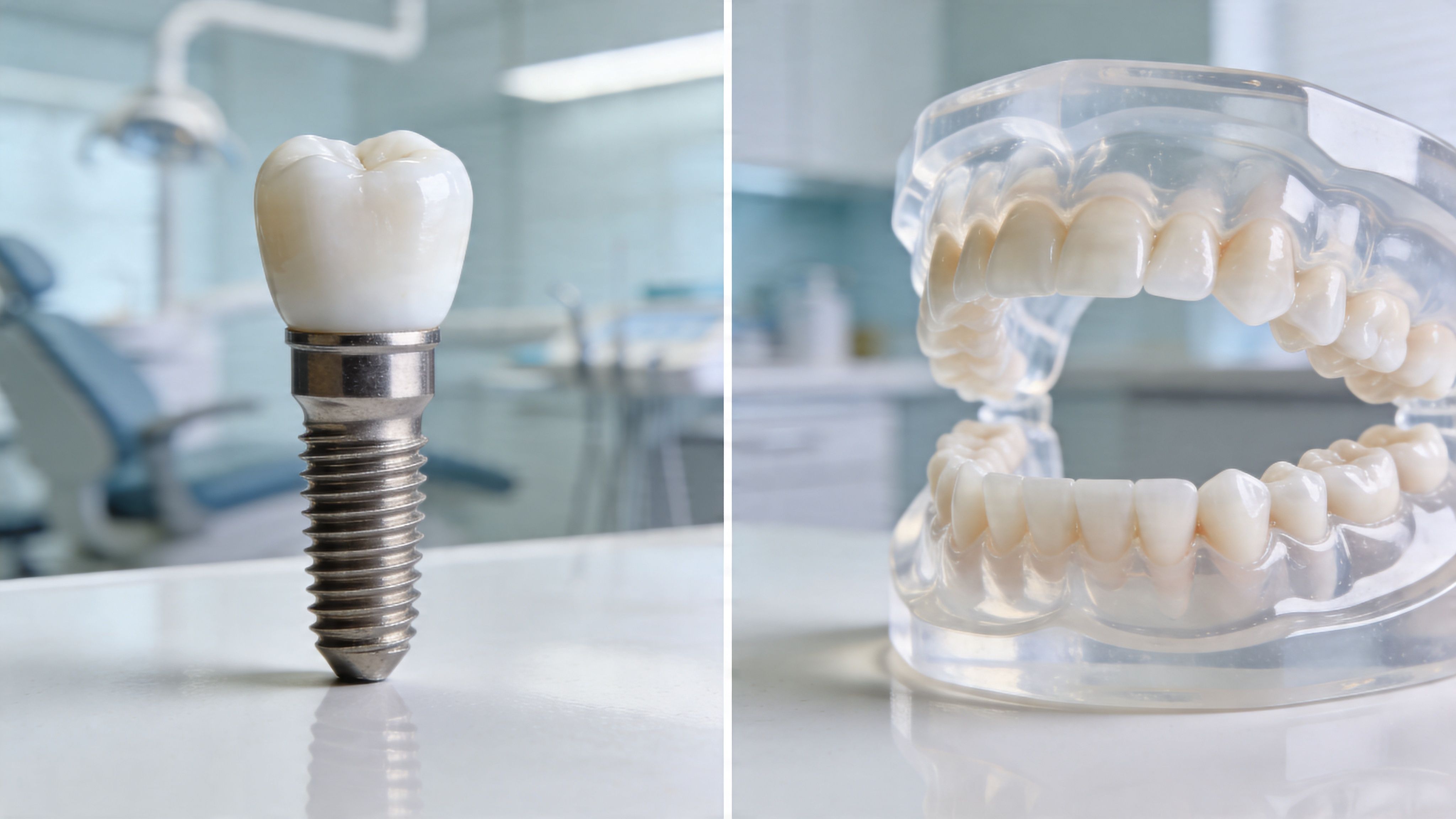
A dental implant replaces the root of the tooth, not just the visible part. That matters because a strong foundation is what gives the restoration its stability.
When the implant integrates with the jawbone, it creates support that traditional removable options can't match. In daily life, that usually means a bite that feels more secure and a smile that doesn't need to come in and out.
What patients usually want to know: Will this still be working years from now, or will I be doing this all over again?
That's the right question to ask.
Implants are often the best fit for adults who want a fixed option for a missing tooth, multiple missing teeth, or a full-arch restoration. They're also part of a bigger restorative plan for patients who may need tooth extraction, crowns, bridges, or other treatment before the final implant is placed.
What makes an implant last in real life
Longevity isn't just about the implant itself. It's about the conditions around it.
Several things have to go right:
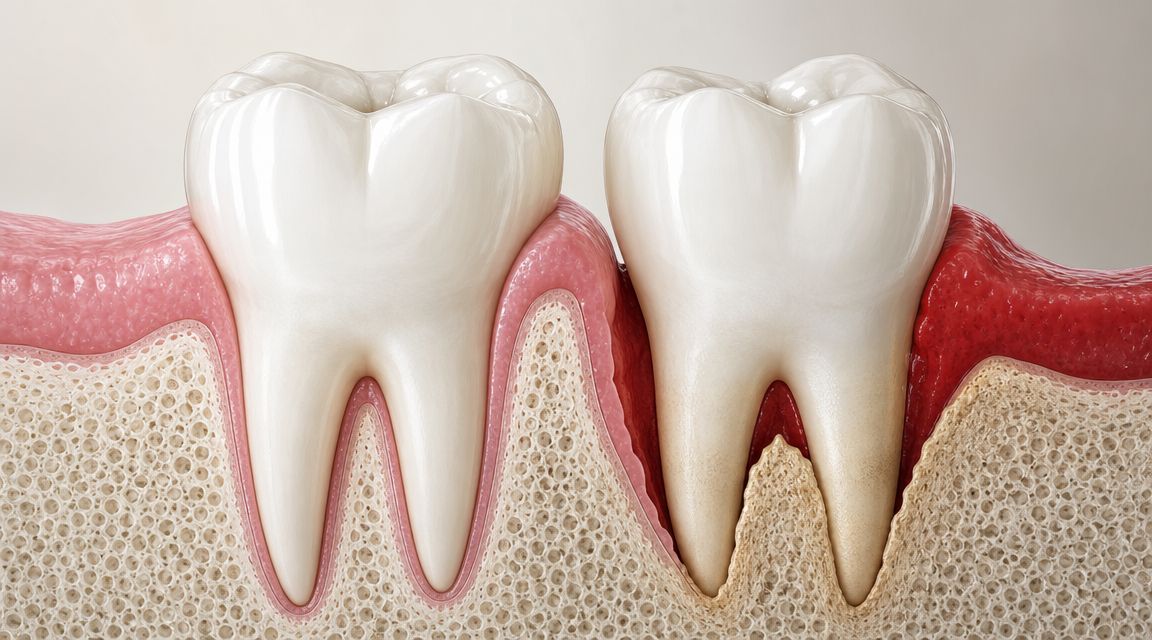
- Healthy gums: Inflamed or infected gum tissue makes long-term stability harder.
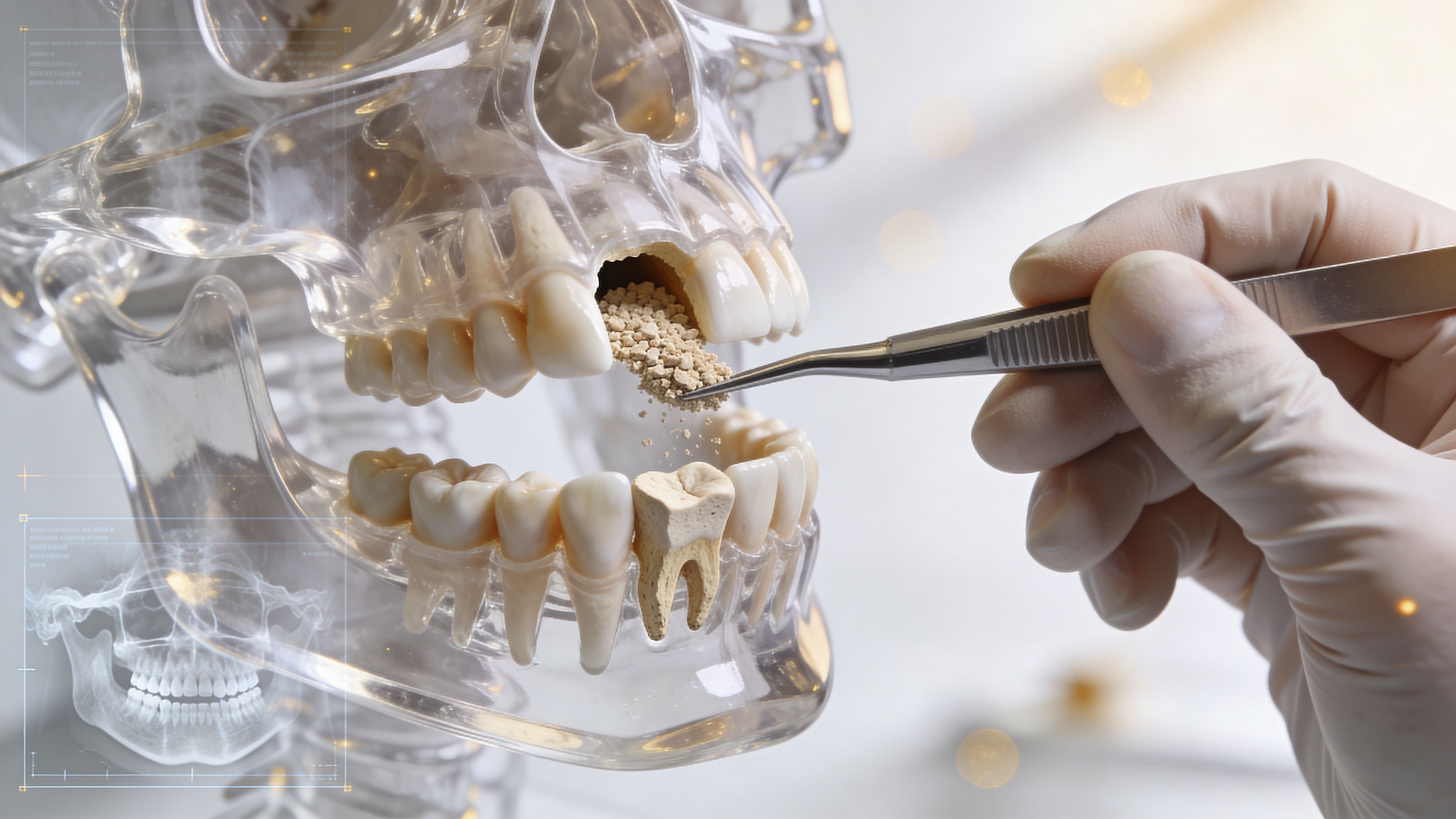
- Strong bone support: Bone quality affects how well the implant starts and how well it holds.
- Accurate planning: Position, angle, and bite design all matter.
- Ongoing maintenance: Implants need regular cleaning and exams, just like natural teeth.
Patients often assume the main decision is whether to get an implant or not. In practice, the bigger difference is how carefully the case is planned and how consistently the implant is maintained.
Why local follow-up matters
If you're looking for a dentist near me in Austin or Georgetown, convenience matters for more than scheduling. Implant treatment works best when your exams, imaging, restoration design, and follow-up care are all easy to keep up with.
That's especially true if you also need routine dental care, cleaning and exams, dental x-rays, or support from a practice that handles both restorative and cosmetic treatment. The less fragmented your care is, the easier it is to protect the result for the long haul.
Dental Implant Survival Rates A 20-Year Outlook
A patient in Austin who is comparing implants with a bridge or denture usually asks the same practical question first. Will this still be working for me 10, 15, or 20 years from now?

In real practice, dental implants have a long track record. Many remain stable and functional for decades. At 20 years, a meaningful majority are still serving patients well, especially when placement, bite design, and maintenance were handled carefully from the start.
That long view matters to patients because an implant is not just a replacement tooth on top. It is a replacement root in the bone. That foundation usually gives implants a longer service life than options that rest on the gums or rely on neighboring teeth for support.
What “survival rate” actually means
Survival rate is a technical term, but the patient-focused meaning is simple. It asks whether the implant itself is still in place and usable years later.
It does not mean every part of the restoration will look exactly the same forever. The implant post may stay stable for decades while the crown, bridge, or denture attached to it needs adjustment, repair, or replacement from normal wear. That distinction is important because patients are often judging the whole treatment by one number.
| Part of treatment | What patients usually want to know |
|---|---|
| Implant survival | Is the implant still stable in the bone? |
| Day-to-day function | Can I chew, smile, and speak with confidence? |
| Restoration wear | Could the crown or bridge need future repair or replacement? |
Why long-term results vary from office to office
Implants are durable, but they are not all planned the same way.
At 3D Dental, we use 3D CT scans before surgery to study bone shape, density, nerve position, and the angle of load on the final restoration. That changes long-term predictability in a practical way. Better planning reduces the chance of placing an implant in a position that creates unnecessary stress over years of chewing.
Our in-house lab also helps. The crown or full-arch prosthesis can be designed with closer control over fit, bite balance, and material choice. Those details affect wear patterns, screw loosening, and overload. Over 20 years, small design decisions can make a large difference.
Patients who want more detail can review our discussion of dental implant success rate and what affects it over time.
Why implants often hold up better than bridges and dentures
A bridge can be an excellent treatment in the right case, but it depends on the health and strength of the teeth next to the gap. A denture can restore appearance and some function, but it sits on tissue that changes over time. An implant is anchored in bone, which gives it a different kind of support under chewing pressure.
That is one reason implants are often the better long-term value, even though the upfront investment is higher. Patients are not only paying for a tooth replacement. They are paying for stability.
A realistic 20-year expectation
Patients should expect durability, not perfection.
Over a 20-year period, the implant itself may continue to function well while the visible restoration shows wear, especially in patients who grind their teeth or put heavy force on the bite. In my experience, the strongest long-term cases are the ones where the surgery, lab work, and follow-up care were designed together from day one.
The practical takeaway is straightforward. Dental implants are one of the longest-lasting ways to replace missing teeth, and the odds improve when advanced imaging, precise restoration design, and consistent maintenance are built into the treatment from the beginning.
Key Factors That Influence How Long Your Implants Last
Two patients can receive implants made from the same material and still have very different long-term results. In practice, the difference usually comes down to planning, bite forces, healing conditions, and maintenance over the years.
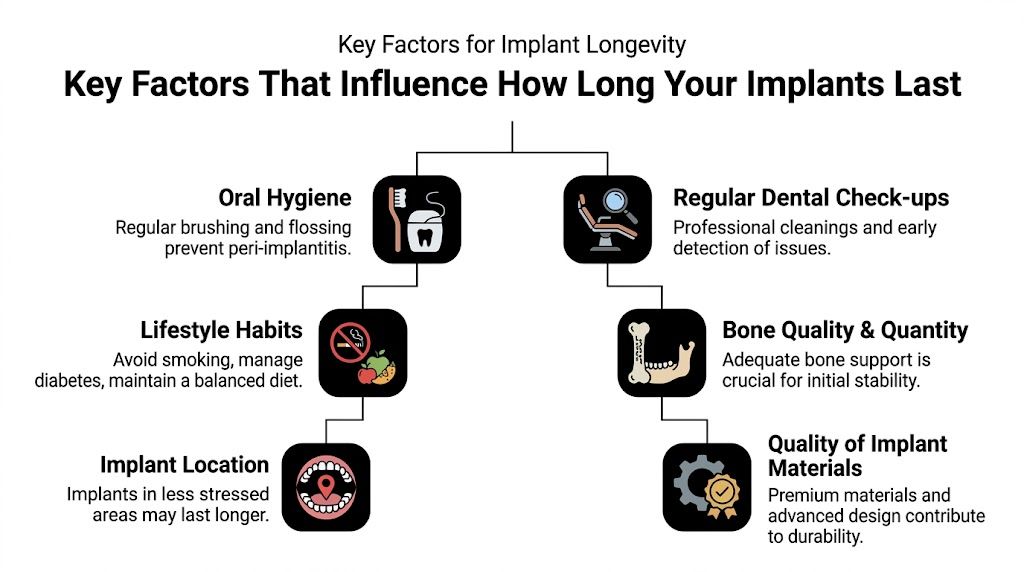
Bone quality sets the foundation. One long-term review reported 97.6% survival in Type I dense bone compared with 88.8% in Type IV soft bone, which helps explain why pre-surgical evaluation has such a large effect on outcome (bone density and implant outcomes).
Bone quality changes the starting point
An implant needs enough bone volume and density to heal under stable conditions. Dense bone usually gives better initial fixation. Softer or thinner bone can still support an implant, but the case requires more control over implant size, position, and healing strategy.
At 3D Dental, we use 3D CT imaging to check bone height, width, density, and nearby anatomy before surgery. That allows treatment planning around the actual site instead of estimates from a two-dimensional image. For patients in Austin and Georgetown, that often means fewer surprises, better implant positioning, and a restoration designed to last under real chewing forces.
Daily habits have a direct effect on longevity
Implants do well in a healthy mouth. They struggle in an inflamed one.
The patterns that matter most are straightforward:
- Oral hygiene: Plaque around the implant can inflame the gums and contribute to bone loss.
- Smoking: Smoking reduces blood flow and makes healing less predictable.
- Diabetes control: Poorly controlled blood sugar can slow healing and increase tissue problems.
- Grinding and clenching: Heavy bite force can wear crowns, loosen screws, or overload the supporting bone.
Bruxism deserves special attention because many patients do not realize they grind until they start breaking fillings, chipping teeth, or waking with jaw tension. In implant cases, that force does not disappear. It transfers to the crown, abutment, and bone interface. A night guard, bite adjustment, and material selection can make a meaningful difference in how long the restoration holds up.
Placement precision affects how the implant handles force
Implants last longer when the surgical position matches the final restoration. If the angle is off or the depth is wrong, the crown may end up carrying force in a way the bone and hardware were not meant to handle.
That is why restoration-driven planning matters. The implant should be placed for the final tooth position, gum contours, and bite relationship. At 3D Dental, that planning is strengthened by our in-house lab workflow, because the surgical and restorative sides of the case are built together rather than treated as separate steps. Patients benefit from a more controlled fit, more predictable esthetics, and fewer mechanical compromises.
Three planning details usually have the biggest effect:
Site evaluation before implant selection
The bone and soft tissue need to be measured first so the implant diameter, length, and position match the case.Restorative design before surgery
The crown or bridge design should guide implant placement, not be forced to adapt to a poor position later.Bite management after healing
The restoration has to contact evenly and avoid taking excessive load in one area.
Maintenance visits protect the investment
A stable implant still needs follow-up. Small problems are much easier to correct when they are found early, before bone loss, screw loosening, or gum inflammation become advanced.
Regular maintenance visits help us check tissue health, clean around areas patients cannot always reach well at home, and monitor wear patterns. The reason this is significant is simple. Implant complications often begin without clear indications, and many patients feel no pain during the early stages.
What works and what doesn't
Reliable long-term results usually follow the same pattern.
| Works well | Usually creates problems |
|---|---|
| Detailed imaging before surgery | Limited diagnostics and rushed planning |
| Good home care around the implant | Plaque buildup at the gumline |
| Regular exams and professional maintenance | Waiting until something feels loose or sore |
| Managing grinding and bite overload | Ignoring clenching, fractured porcelain, or worn bite surfaces |
Patients searching for cosmetic dentist near me often focus first on how the final tooth will look. That is understandable. With implants, though, appearance lasts best when the bone, bite, and restoration design are handled correctly from the start.
Single Tooth Implants vs Full-Arch Solutions Longevity
A single implant and a full-arch implant restoration are both built on the same basic idea. They replace missing teeth with anchored support in the jaw. But they don't wear the same way, and they don't ask the same things from the materials on top.
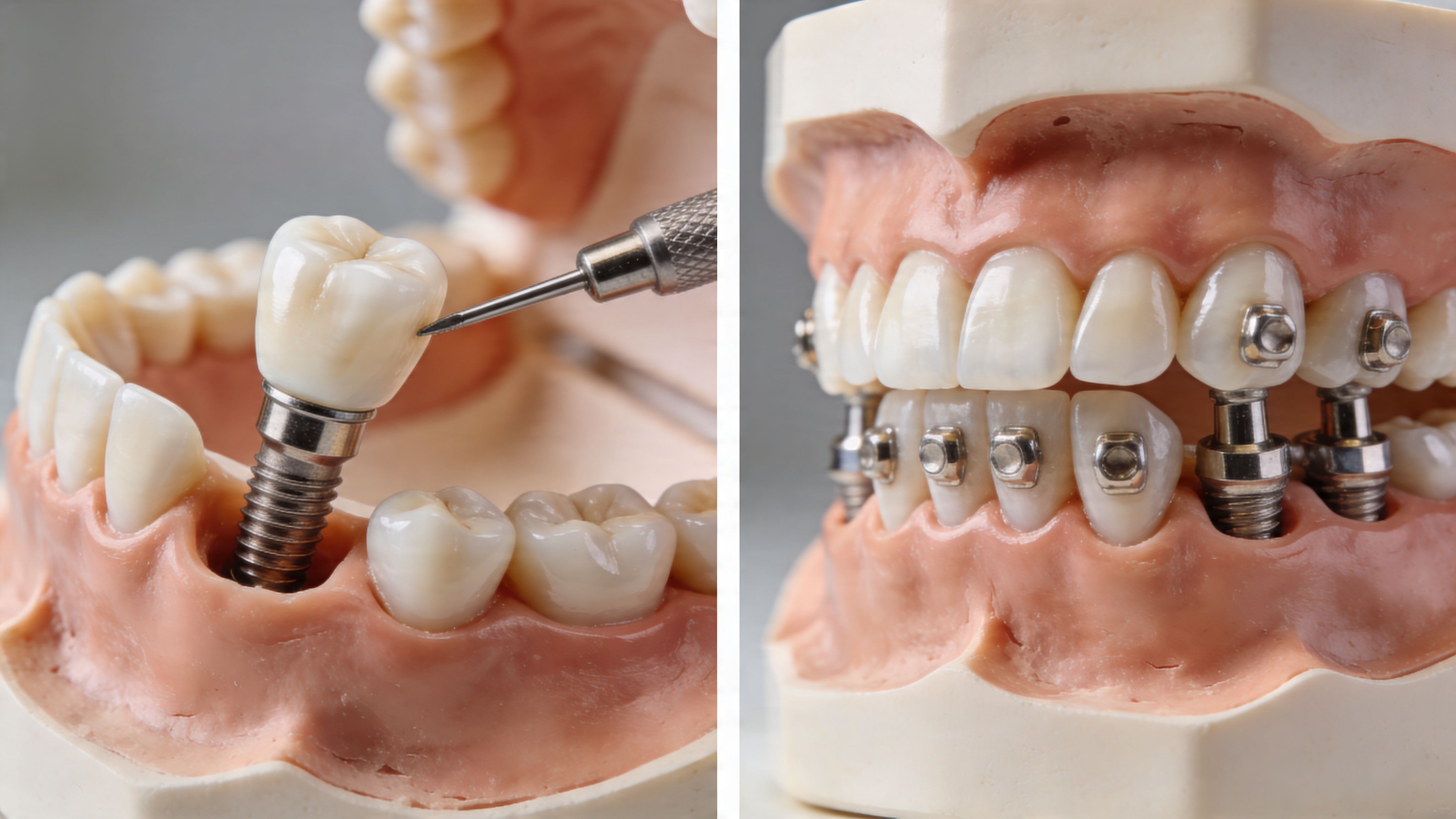
A major review found that the titanium post often lasts 25+ years, while the abutment and crown typically last 10 to 15 years. For All-on-4 or implant bridges, 50 to 80% of prosthetic crowns may require replacement within 15 to 20 years due to wear (implant component lifespan review).
Single tooth implants tend to be simpler to maintain
A single implant usually replaces one missing tooth with one implant post and one crown. That setup is mechanically straightforward.
If the crown wears out or chips years later, the underlying implant may still be perfectly stable. In many cases, the visible part can be replaced without starting over.
That simplicity gives single-tooth implants an advantage in maintenance. There are fewer connected parts and fewer force-distribution issues across an entire arch.
Full-arch cases carry different demands
A full-arch restoration, including All-on-4 style treatment, is often life-changing for patients with many failing or missing teeth. It restores bite strength, smile support, and daily confidence.
But full-arch restorations are more complex. Several implants support a larger prosthesis, and the prosthesis takes repeated force across a much wider area.
That doesn't make the option less durable. It means patients should expect a different maintenance profile.
| Feature | Single tooth implant | Full-arch solution |
|---|---|---|
| Main replacement | One missing tooth | An entire upper or lower arch |
| Usual wear point | The individual crown | The prosthetic teeth and larger restoration |
| Maintenance style | Focused and localized | Broader monitoring of bite, screws, and prosthetic wear |
| Repair pattern | Often limited to one tooth unit | May involve larger restorative updates over time |
The post and the prosthetic are not the same thing
Patients sometimes get confused. They hear that implants can last decades, then assume every attached part lasts exactly as long.
That usually isn't how it works.
The implant post in the bone is the long-term anchor. The crown, bridge, or full-arch prosthesis is the working surface that handles chewing, clenching, heat changes, and daily wear. That visible layer often needs attention sooner.
The better question isn't only “Will the implant last?” It’s also “Which part might need service first?”
Which option is “better” for longevity
Neither is automatically better in every case. The right answer depends on how many teeth are missing, how the bite functions, how much bone support is available, and what kind of maintenance the patient can commit to.
A single implant is often easier to service because it's isolated. A full-arch case may involve more future prosthetic maintenance, but it can still be the best long-term choice for someone with widespread tooth loss.
Patients looking for restorative dentistry in Austin or Georgetown often need this distinction explained clearly. The goal isn't to promise that every part lasts forever. The goal is to build the strongest foundation possible and make future maintenance predictable.
How to Care for Your Implants for Lifetime Results
Good implants still need good habits. The patients who keep their implants looking and feeling stable over the long term usually do a few simple things consistently.

Daily care doesn't have to be complicated. It just has to be thorough.
What to do at home every day
Brush around the implant carefully, especially where the gum meets the restoration. That margin is where inflammation usually starts if plaque sits undisturbed.
A simple home routine often includes:
- Soft brushing: Use a soft toothbrush and clean the gumline gently, not aggressively.
- Between-the-teeth cleaning: Floss, implant floss, or other cleaning aids can help reach areas a brush misses.
- Consistent timing: Skipping several nights in a row is where trouble begins, not missing one perfect cleaning session.
- Awareness of changes: If the tissue looks red, puffy, or bleeds more easily, don't ignore it.
Patients who want more detailed day-to-day guidance can review this practical article on how to care for dental implants.
Professional care matters even if nothing hurts
Implants can develop problems unnoticed. You may not feel pain when gum inflammation or early bone changes begin.
That's why regular recall visits matter. Professional cleanings, bite checks, and periodic imaging help catch wear, looseness, and tissue changes before they threaten the restoration.
A common mistake is assuming an implant doesn't need much attention because it isn't a natural tooth. In reality, the surrounding gums and bone still need monitoring.
If something feels slightly “off” around an implant, waiting rarely improves it.
A visual walkthrough can help patients understand the cleaning approach and what healthy implant care looks like over time.
The overlooked issue is grinding
Bruxism is one of the most common reasons an implant crown wears out sooner than expected. Reported guidance notes that teeth grinding can cut the life of an implant crown down to 5 to 10 years, and custom night guards are often used to protect the restoration. The same source also notes that modern 3D-printed crown materials can improve durability by 30 to 50% compared with traditional porcelain (bruxism, crown wear, and modern materials).
That doesn't mean every grinder will damage an implant quickly. It means the bite has to be managed, especially at night.
Patients often know they clench because they wake up with jaw tension, morning headaches, or worn natural teeth. If that's happening, it's worth addressing before or after implant treatment rather than hoping it won't matter.
Warning signs that need an exam
Call your dentist if you notice any of the following around an implant:
- Bleeding at the gumline: Occasional irritation can happen, but repeated bleeding isn't something to dismiss.
- A change in bite: If the tooth starts hitting first or feels high, that can create overload.
- Looseness or movement: The crown may be loose, or the issue may be deeper. Either way, it needs evaluation.
- Persistent tenderness: Ongoing soreness around the implant or gum tissue deserves a closer look.
- Chipping or wear: Small damage often leads to bigger stress if it's left alone.
For patients also seeking cleaning and exams, new patient exams, or regular preventive care, keeping those visits on schedule is one of the most effective ways to protect the investment.
Your Implant Journey at Our Austin and Georgetown Offices
Most patients feel better about implants once they know how the process works. The experience is usually more structured and more personalized than they expected.
It starts with diagnosis, not guesswork
The first visit is about deciding whether an implant is the right treatment and what the site can realistically support.
That exam typically includes a clinical evaluation, digital imaging, and a discussion about the missing tooth, the bite, the gums, and the surrounding teeth. If a patient is also dealing with a damaged tooth, infection, or failing dental work, those issues need to be addressed before the final implant plan is set.
For some patients, the path includes tooth extraction first. For others, the implant replaces a tooth that's already been missing for some time.
Planning the final tooth before the procedure
Strong implant treatment starts backward. The doctor plans the final restoration first, then places the implant to support that result.
This approach matters because implant placement isn't just surgical. It also has to work aesthetically and functionally. The tooth has to emerge from the gum in the right position, fit the bite, and be easy to clean.
A modern office with 3D CT imaging, digital scanners, and an in-house lab can make that planning process more precise. It also helps shorten delays between the design phase and the final restoration.
The best implant cases usually look simple to the patient because the planning was detailed behind the scenes.
The placement and healing phase
Once the plan is complete, the implant is placed in the jaw. After placement, the body needs time to heal and integrate with the implant.
During healing, patients receive instructions on cleaning, eating, and protecting the area. This stage is where following directions matters. Healing tends to go more smoothly when the site is kept clean and isn't overloaded too early.
Some patients are replacing one tooth. Others are planning larger restorative care such as multiple implants or full-arch treatment. The steps differ, but the principle stays the same. Build a stable foundation first, then finalize the restoration.
What follow-up feels like for the patient
After healing, the final crown, bridge, or arch is delivered and adjusted. The patient should leave with a restoration that looks natural, feels stable, and fits the bite comfortably.
Follow-up care doesn't stop at delivery. Implant dentistry works best when the patient has a clear maintenance plan for routine checkups, professional cleanings, and any bite adjustments if needed later.
For many adults looking for a dentist near me in Austin or Georgetown, that's an important part of the decision. They want one office that can handle the full process, from diagnosis to restoration to ongoing maintenance, without sending them in several directions.
Frequently Asked Questions About Dental Implant Longevity
Can a dental implant really last a lifetime
Yes, it can. The best way to say it is that implants are designed as a long-term solution, and some remain functional for decades. Whether one lasts a lifetime depends on bone support, oral hygiene, bite forces, general health, and regular maintenance.
Does the implant itself wear out, or is it usually the crown
It's often the visible restoration that needs service first. As covered earlier, the implant post in the bone is the long-term anchor, while the crown or prosthetic teeth take the daily wear from chewing and clenching.
Are implants better than bridges or dentures for long-term value
In many cases, yes. Implants tend to last longer and offer a more stable feel. They also preserve support in a way removable options don't. That said, “better” still depends on the condition of the mouth, the number of missing teeth, and whether the patient is ready for the required care.
What are the earliest signs something may be wrong
The most common early signs are subtle. Watch for bleeding around the implant, bad taste, puffiness, tenderness, a crown that feels loose, or a bite that suddenly feels different.
Those signs don't always mean the implant is failing. They do mean the area should be examined promptly.
If a crown breaks, does the whole implant have to be replaced
Not usually. In many cases, the implant itself remains stable and only the crown or another prosthetic component needs repair or replacement. That's one reason regular exams are useful. Small restorative problems are easier to fix when they're found early.
Is an implant still a good option if I grind my teeth
Often, yes, but the treatment plan has to account for that habit. Grinding can put extra stress on the crown and bite, so many patients need a protective night guard and closer follow-up.
How often should implant patients come in
The right schedule depends on the patient's gums, home care, bite, and history. In general, implant patients do best when they keep routine preventive visits and don't wait for symptoms to appear before coming in.
If you're comparing options for missing teeth, want a second opinion, or are searching for dental implants near me, cosmetic dentist near me, or a trusted dentist in Austin, TX or dentist in Georgetown, TX, the smartest next step is a consultation focused on your bone support, bite, and long-term goals.
If you're ready to replace a missing tooth or explore full-arch treatment, schedule a consultation with 3D Dental. With advanced imaging, digital planning, an in-house lab, and offices serving Austin and Georgetown, the team can help you choose an implant solution built for long-term function, comfort, and confidence.
Ready to get started?
Schedule a free, no obligation consultation with our team and see what's possible for your smile!
Georgetown
- Mon-Thurs8:30am-5pm
- Fri8am-3:30pm
- Sat-SunClosed
Austin
- Mon-Tues8am-5pm
- Wed-Thurs9am-6pmFri8am-2pm
- Sat-SunClosed